
ADVERSE PREGNANCY OUTCOMES
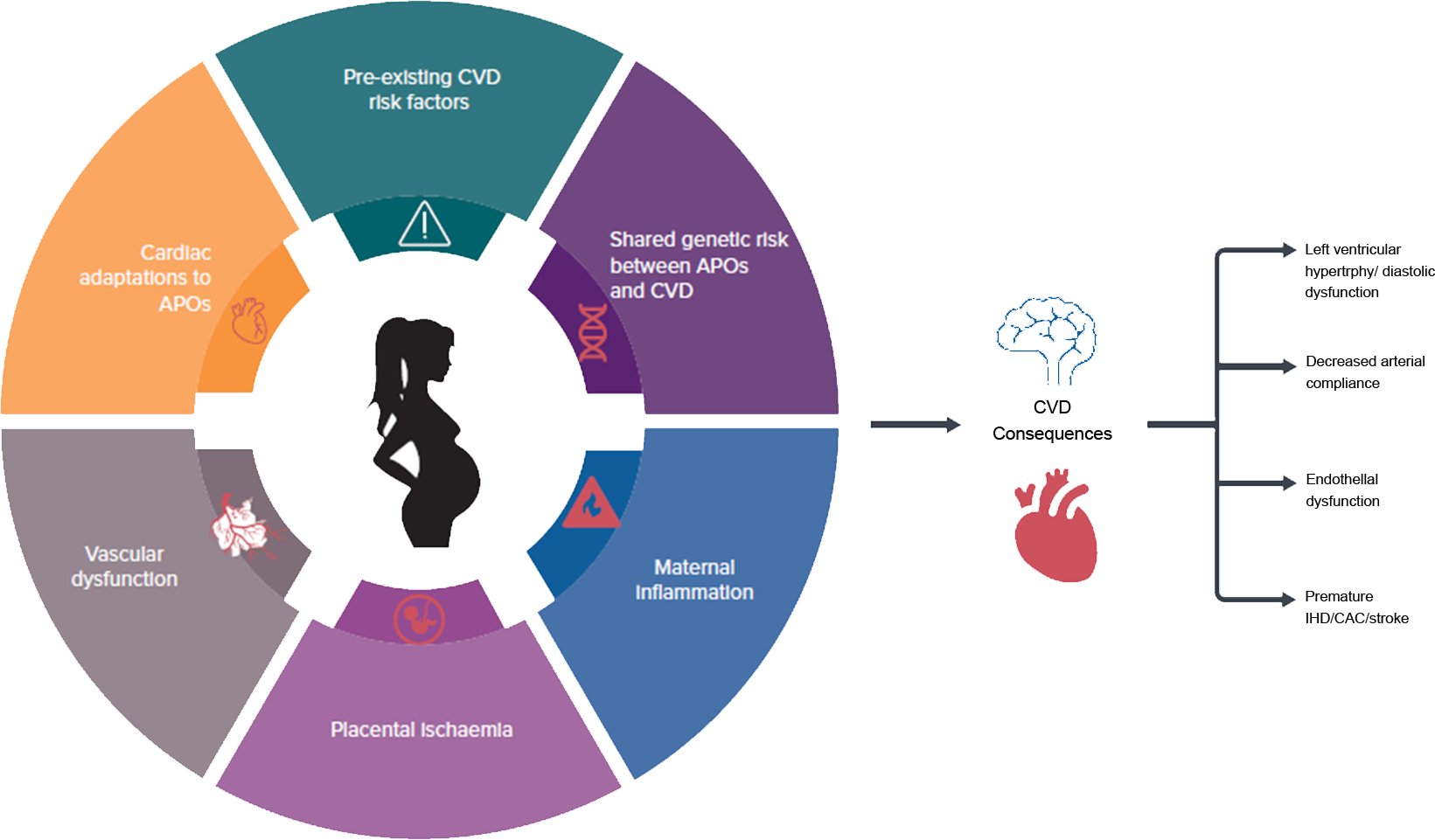 The burden of adverse pregnancy outcomes is substantial in both developed and developing countries (Lee et al, 2013; Beck et al, 2010; Blencowe et al, 2012). More than 60% of preterm births take place in south Asia and sub-Saharan Africa (Blencowe et al, 2012). APO is a complex, multi-factorial, physiological outcome in women, and despite decades of research, a clear causal mechanism for these adverse outcomes has not been established.
The burden of adverse pregnancy outcomes is substantial in both developed and developing countries (Lee et al, 2013; Beck et al, 2010; Blencowe et al, 2012). More than 60% of preterm births take place in south Asia and sub-Saharan Africa (Blencowe et al, 2012). APO is a complex, multi-factorial, physiological outcome in women, and despite decades of research, a clear causal mechanism for these adverse outcomes has not been established. Objectives
- Investigate biochemical and immunological markers associated with adverse outcomes of pregnancy.
- To possibly generate a new hypothesis based on models combining the ongoing omics and the above markers.
- To utilize the dataset for population-specific analysis and address unique local health problems.
- Come up with hypotheses for newer projects based on the combined datasets.
SEPSIS
 While India has made significant progress for reducing under five mortality in the last decade, efforts are still being undertaken by the government to achieve the 3rd Sustainable Development Goal of
under-five mortality of 25 per 1000 live births by 2030. As per the National Health Policy, the effort is also to reduce
neonatal mortality to 16 by 2025 and to address malnutrition by reduction of 40% in prevalence of stunting of under 5
children by 2025.
While India has made significant progress for reducing under five mortality in the last decade, efforts are still being undertaken by the government to achieve the 3rd Sustainable Development Goal of
under-five mortality of 25 per 1000 live births by 2030. As per the National Health Policy, the effort is also to reduce
neonatal mortality to 16 by 2025 and to address malnutrition by reduction of 40% in prevalence of stunting of under 5
children by 2025. While neonatal mortality rate has declined from 38 in 2000 to 23.5/ 1000 in 2017, we are still far from achieving the target by 2025. If neonatal mortality and malnutrition are to further decline, newer modalities for managing neonatal infections (septicaemia, meningitis and pneumonia) have to be introduced. Low birth weight accounts for 40-80% deaths in neonates. Neonatal sepsis encompassed septicaemia, pneumonia, meningitis, osteomyelitis, arthritis and urinary tract infections and does not have a common case definition, especially for Low- and Middle- Income Countries (LMICs). In case of sepsis, infection spreads rapidly which leads to severe disease and death in low birth weight neonates and thus prevention of infection would lead to decrease in neonatal morbidity and mortality. However, there are no preventive interventions for neonatal sepsis currently. Probiotics are currently being considered a useful intervention for growth, sepsis in infants. While exact mechanism of action of probiotics is not known, they are assumed to protect neonates from developing sepsis by improving gut barrier function, competitive exclusion of pathogens, modification of host immune responses, augmentation of immunoglobulin A (IgA) mucosal responses, and enhancement of enteral nutrition that inhibits the growth of pathogens and aids in upregulation of immune responses. Center for Public Health Kinetics is a part of an ICMR funded large, multicentric, parallel-arm, placebo-controlled study using a mix of 8 strains of bacteria to conclusively evaluate the role of probiotic in the prevention of neonatal sepsis.
